
Psoriasis Before and After Treatment: Recommendations for Keeping a Chronic Condition Under Control
Contents
Psoriasis is a complex illness manifesting with the characteristic scaly, red skin plaques. Most patients start having symptoms between the ages of 15 and 30, though it is rare before age 10. The condition strikes when people are in the prime of life. Understandably, some have a hard time coping with it.

Psoriasis is incurable, but modern medicine has found ways to manage the symptoms effectively and induce long remissions. This article explains the different clinical forms of psoriasis and what patients can expect before and after treatment. It also highlights the importance of the patient-doctor partnership in keeping this chronic condition under control.
What Are the Types of Psoriasis?
The clinical forms of psoriasis differ by time course, as well as lesion distribution and physical characteristics. Some affect certain age groups more than others. These conditions are explained below.
Psoriasis Vulgaris
Psoriasis vulgaris is the most common type, seen in about 90% of patients. It is also known as “chronic plaque psoriasis” because of its lifelong, waxing and waning course and the presence of the classic psoriasis plaques.
The lesions are raised and red, with borders easily distinguishable from the surrounding skin. Silvery or white scales cover the surface. The plaques are itchy and may coalesce without treatment. Psoriasis vulgaris lesions usually appear on the trunk, scalp and outer joint (extensor) surfaces.

Inverse Psoriasis
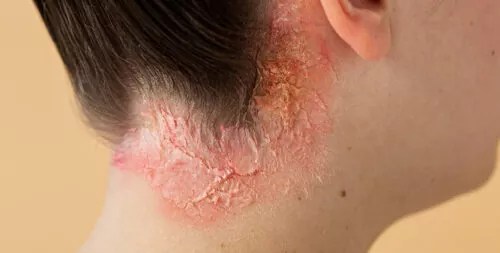
Inverse psoriasis is otherwise known as “flexural psoriasis” because of its appearance in the inner joint (flexural) surfaces. It can also affect the major skin folds, such as the armpits, groin region and neck.
Inverse psoriasis lesions are less scaly and tend to look shiny because they appear in areas where oil glands abound. Less sweating can be observed in the affected locations.

Guttate Psoriasis
This type of psoriasis affects mostly children, adolescents and young adults. It occurs as an eruption of red, small lumps 0.5-1.5 cm in diameter, usually on the limbs and upper trunk. Streptococcal throat infection is thought to trigger its appearance, although antibiotics do not shorten its duration.
This skin condition may resolve even without treatment, but about one-third of patients develop chronic plaque psoriasis later in life.
Psoriasis vulgaris patients may also see guttate lesions alongside chronic plaques.

Small Plaque Psoriasis
This psoriasis type presents with guttate lesions, though they develop gradually and affect older patients. Thicker, scalier and larger lesions may appear. Small plaque psoriasis is more common among patients of Asian heritage.

Sebopsoriasis
The plaques of sebopsoriasis are also red but have greasy scales. This type usually affects oil gland-rich areas like the scalp, skin folds, glabella (the region between the eyebrows), center of the face, etc.
Sebopsoriasis is sometimes hard to differentiate from seborrheic eczema. Like the latter, it is believed to be triggered by a fungal infection and responds to antifungals.
Napkin Psoriasis
This rare form of psoriasis affects infants 3-6 months old. It appears suddenly, first in the diaper (napkin) area, spreading to the trunk and limbs later. It may sometimes involve the face.
The initial lesions are small, scaly, red lumps that can merge and grow within days. The condition responds well to standard treatments and disappears after 12 months of age.

Linear Psoriasis
The psoriatic lesions in this rare clinical type are linear in form, appearing on the limbs and trunk. It is more frequent among adults than children. Linear psoriasis also responds readily to therapy.

Pustular Psoriasis
In pustular psoriasis, small, pus-filled lesions (pustules) erupt on the surface of chronic plaques. The pus normally does not contain microbes, so it is “sterile,” although bacterial infection of ruptured pustules can occur.
This clinical form of psoriasis may be localized or generalized.
Localized pustular psoriasis affects only certain areas, such as the hands and feet.
Meanwhile, generalized pustular psoriasis lesions are more widespread. The von Zumbusch variant manifests with fever and is potentially fatal.

Erythrodermic Psoriasis
Erythrodermic psoriasis is an acute exacerbation of the disease, and it can evolve on top of any other type of psoriasis. The diffusely red, scaly lesions occupy at least 75-90% of the total body surface area (TBSA). The condition impairs the body’s ability to regulate temperature, so patients may become extremely cold or hot. Erythrodermic psoriasis can cause heart failure, so it is treated as an emergency.

The different psoriasis types are further classified as mild, moderate, or severe, depending on the extent of skin involvement.
Mild psoriasis involves less than 10% TBSA. Moderate psoriasis affects 10-30% TBSA, while severe psoriasis involves greater than 30% TBSA. One way of estimating the area of skin affected is by using the patient’s hand as a measurement guide. The size of the palm, including the fingers, is equivalent to 1% TBSA.
The psoriasis area and severity index (PASI) is another grading scale doctors use to classify the disease based on severity. But it is beyond the scope of this discussion. Grading is important in treatment planning, as some therapies are more aggressive than others.
What Is the Main Cause of Psoriasis, and What Makes It Act Up?
The cause of psoriasis is unknown, though it has strong genetic and autoimmune features. It tends to run in families and responds to immunosuppressants.
Meanwhile, environmental factors are thought to contribute to disease onset and exacerbation. The ones with the strongest evidence in the literature include the following:
Infection
As previously mentioned, some types of psoriasis are associated with infections. Strep infection is the most widely implicated in guttate psoriasis. But some individuals with psoriasis vulgaris also experience a breakout after such an illness.
Others found to have a strong connection with psoriasis flares are Staphylococcus aureus (normally present in the skin), some fungal species and HIV.
Medications
Drugs likely to exacerbate psoriasis include the following:
- Antimalarials, which may be prescribed to travelers and patients with autoimmune disease
- Beta-blockers, gemfibrozil, and ACE inhibitors, which are commonly given to individuals with hypertension and heart disease
- Lithium, a mood disorder medication
- Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and aspirin
- Interferons, given for chronic viral illnesses and immune-driven conditions
- Imiquimod, an immunosuppressant used in treating various skin disorders
Drug-related psoriasis may present with either localized or widespread lesions. Many pustular and erythrodermic psoriasis cases are thought to be due to prior medication use. The abrupt cessation of steroids and other immunosuppressants has also been implicated in the development of potentially fatal psoriasis.
Skin Trauma
Trauma to the skin can give rise to new psoriatic lesions—a skin reaction known as the “Koebner phenomenon.” Radiotherapy, burns, cuts, UV radiation, skin irritation, scratching, etc. can all cause Koebnerization.

Air Pollutants
Psoriasis patients often have higher blood cadmium levels than the general population. This heavy metal makes its way into the air from burning fossil fuels and waste, metal mining and steel plant fumes.
Sun Exposure
The sun is a natural source of UV radiation. Excessive sun exposure can burn the skin and produce new lesions.
Vaccines
Psoriasis breakouts are more likely after influenza and BCG vaccination. Flares have also been documented after using some COVID-19 vaccine formulations, specifically Moderna and AstraZeneca.
Vaccines activate the immune system, which is thought to increase a patient’s risk of developing new lesions.
Lifestyle
Among lifestyle factors, cigarette smoking has the strongest link to psoriasis exacerbation. Moreover, the number of cigarettes a person has smoked over time—estimated in pack-years—directly correlates with disease duration. Smoking is also the most likely to cause pustular psoriasis.
By comparison, alcohol drinking is less associated with psoriasis flares. However, alcohol consumption reduction has been linked to symptom improvement in psoriasis patients. Additionally, chronic heavy alcohol use has been associated with increased psoriasis mortality risk.
Meanwhile, there is not enough evidence linking food to psoriasis exacerbation. But beef, monosodium glutamate, gluten and nightshade plants have been implicated in the literature.

Obesity by itself does not trigger psoriasis breakouts. However, it can make people living with this skin condition more prone to diabetes mellitus and cardiovascular disease. Obese patients are also more likely to develop severe psoriasis.
What Do BHSkin Dermatology Specialists Do for Psoriasis?
Our skin care experts at BHSkin Dermatology use various therapies scientifically proven in treating psoriasis. We cover many of them in our article on psoriasis treatment options. But we discuss them briefly below:
Topical Medications
Topical agents are the first line of treatment for mild to moderate psoriasis. They are also used in combination with other forms of therapy for severe plaque psoriasis.
Most topical psoriasis treatments suppress the skin’s abnormal cell growth, immune response or both. They include topical steroids, vitamin D-like drugs, vitamin A-like agents and skin cell growth inhibitors.
Exfoliants like salicylic acid reduce excessive skin thickness, making them useful in treating chronic plaques and mild scalp psoriasis. Emollients protect the skin from further inflammation by preventing dryness and cracking.

Light Therapy
Light-based procedures used on psoriasis include PUVA phototherapy, UVB phototherapy and excimer laser treatment. Ultraviolet radiation inhibits the skin’s immunity and erratic growth and does not affect vital organs. Skin cancer is one of the long-term risks of these treatments, but it may be minimized by scheduling the regimen annually.
UVB phototherapy is best for severe psoriasis and milder cases resistant to topical treatment. Nail and scalp psoriasis also respond to this modality.
PUVA phototherapy, which has a higher risk of skin cancer, is reserved for patients with more aggressive psoriasis symptoms, e. g. generalized pustular psoriasis.
Excimer lasers are in the same light spectrum as UVB radiation. Dermatologists use them to treat small psoriasis plaques.

Systemic Therapy
Psoriasis is a disorder of the immune system as much as it is of the skin. Leaving it untreated accelerates the onset of complications, the most common of which is arthritis. Systemic therapy becomes necessary when such complications arise or when the disease becomes aggressive or resistant to topical and light treatments.
Systemic medications commonly prescribed for psoriasis therapy include methotrexate, acitretin, cyclosporine and apremilast. These drugs can induce remission, but doctors carefully control their doses and duration of use to prevent collateral organ damage. Periodic lab tests help monitor organ function during the treatment course.

Biological Response Modifiers
Biologics also have a systemic effect, but they deserve special mention because they are reserved for extremely resistant cases. Examples are secukinumab, etanercept, ustekinumab and infliximab. These agents suppress the immune system on various levels, consequently weakening the body’s immunity. Patients receiving this type of therapy become vulnerable to infection and cancer.

No psoriasis treatment suits every patient. But working with your dermatologist will help you figure out the therapeutic approach most suitable for you.
What Can You Expect During Your Dermatology Consultation for Psoriasis?
BHSkin Dermatology specialists always aim to give the best quality of care, as every patient deserves.
Psoriasis lesions are easy to recognize at first glance, but your doctor’s examination will not stop there. They will listen to your full medical history, which can help determine which treatment is right for you.
After a closer inspection of the exposed lesions, they will ask your permission to examine other areas of your body. Doing so will help them assess the severity of your condition. They will also look for signs of psoriatic arthritis, scalp or nail involvement and other complications. They may photograph the plaques to monitor their appearance before and after treatment.
At the end of the session, they will walk you through your treatment options. Lab tests are usually not necessary unless you require systemic therapy. Rarely, skin cancer can mimic psoriasis. Your doctor may do a biopsy if the diagnosis is doubtful.
What Can You Expect When Receiving Treatment for Psoriasis?
The speed of symptom resolution generally depends on the psoriasis type, the severity of the lesions and the therapy used.
Chronic forms of psoriasis, e. g. psoriasis vulgaris and flexural psoriasis, have a waxing and waning course. That means that after its initial presentation, the disease will enter a stable period, disrupted at times by breakouts.
Topical agents can reduce symptom severity after a few weeks of use. Resistant plaques may be treated with a round of phototherapy or systemic medications. Skin lesions persist in more than half of patients and disappear in the rest. Stable periods may last from one year to several decades.
Guttate psoriasis lesions will disappear within a few weeks or months, even without therapy. But topical steroid creams and emollients help prevent aggravation by reducing inflammation and itchiness. They can also improve the appearance of the lesions after a few weeks. Phototherapy and systemic treatment may be given for widespread involvement or conversion to severe plaque psoriasis.
Patients with active psoriatic arthritis or involvement of the hands and feet will require potent treatments, i. e. phototherapy and systemic drugs. These interventions help reduce pain and relieve immobility, though it may take weeks before patients observe significant improvement.
NSAIDs may be given to people with mild disease who want additional treatments for joint pain. As mentioned previously, these medications can worsen the illness, so doctors discourage their use in severe psoriasis patients. But the latter may benefit from physical therapy.

Erythrodermic and generalized pustular psoriasis are potentially life-threatening and must be treated right away. Unstable patients must be admitted to a hospital and stabilized.
The dermatologist may start several forms of therapy at once to induce quick resolution of symptoms. Most patients observe a marked improvement in a few days, but systemic complications may still arise despite adequate treatment of the skin lesions. So other medical specialists may also be involved in patient care.
The thing is, these scary psoriasis types are rare and more likely to occur in people who have poor control of their chronic symptoms. Furthermore, a trigger is identifiable in more than half of the cases. So you can prevent them by following your dermatologist’s treatment plan and avoiding potential triggers.
Why Is It Important to Treat Psoriasis?
As mentioned above, the immune system plays a huge role in the development of psoriasis symptoms. So patients are innately vulnerable to complications stemming from chronic systemic inflammation, such as:
- Psoriatic arthritis
- Metabolic abnormalities that can result in cardiovascular disease
- Cancer
You can ward off these complications the sooner you treat your symptoms.
Additionally, poorly controlled psoriasis leads to severe exacerbations that are at times resistant to treatment. Staying on top of this illness prevents bad flare-ups and spares you from the harmful effects of aggressive therapies.
Why Should You See a Dermatologist for Psoriasis Treatment?
Board-certified dermatologists are the medical experts to trust in treating psoriasis.
First, they have extensive training in the diagnosis of this disease. Early recognition means timely treatment and better symptom control.
Second, they have advanced knowledge of the various psoriasis remedies. As you can see, some of them have unwanted side effects and must be balanced with each patient’s needs.
An inexperienced provider may prescribe the wrong dose or give it over an inappropriately short or lengthy period. But working with a board-certified dermatologist can spare you from such miscalculations and, consequently, the treatment-related complications.
Third, they have mastery of skin disorders that may resemble psoriasis, one of which is skin cancer. Inaccurate diagnosis can lead to either ineffective or potentially harmful treatments.
At BHSkin Dermatology, our psoriasis specialists are some of the best in California. You’re in the most capable hands when you trust them with your treatments.

The Takeaway
Psoriasis is a complex medical condition with various presentations. Its cause remains poorly understood, though genetic, immune and environmental factors have been implicated in its development.
The disease has a waxing and waning course. More than half of patients have persistent skin lesions, while the rest experience asymptomatic periods of variable duration. Modern psoriasis therapies prevent symptom aggravation, normalize the skin’s immune responses and make flare-ups more manageable. Trigger identification and avoidance have made it possible to prolong remissions.
Finally, psoriasis is an immune-driven disease that must be treated as soon as it surfaces. The best healthcare professional to help you deal with it is a board-certified dermatologist. Only by working with a trusted skin doctor can you get the best chance of restoring your skin’s beauty.
Can’t Get Clearer Skin After a Psoriasis Flare? Talk to LA’s Top Psoriasis Experts
Psoriasis is a multifactorial disorder that may present initially as unsightly blemishes resistant to over-the-counter skincare products. Stubborn skin lesions could be signs of a more serious illness, so it’s best to have them checked and treated by a medical expert as soon as possible.
At BHSkin Dermatology, our award-winning board-certified skin care professionals offer a wide variety of safe and effective psoriasis treatments. Come to our Glendale or Encino clinic or use our virtual portal for a consultation.
Book your appointment today!
Get superior skincare from LA's finest dermatologists
Book the type of an appointment that suits you best.





